
As we are all aware, healthcare is experiencing widespread burnout, with a staggering 77% of healthcare providers reporting varying degrees of stress or burnout. Through extensive research, the KLAS Arch Collaborative, a group of healthcare organizations committed to improving the EHR experience through shared research, standardized surveys, and benchmarking, has identified EHR-related factors as burnout contributors. But the good news is, pinpointing specific EHR experience factors, like tool inefficiency, lack of training, poor proficiency, allows for directed intervention and improvement.
Recently, during the Becker’s Healthcare webinar titled “How Innovative EHR Training can Enhance Clinician Well-being,” experts delved into the realm of EHR training, sharing insights on successful strategies and pitfalls to avoid. Jenna Anderson, representing the KLAS Arch Collaborative, presented illuminating data on optimizing the EHR experience through personalized training and enhanced user engagement. Erin Banaszak provided a compelling glimpse into Froedtert Health’s successful journey in EHR training transformation.
For healthcare systems looking to reinvent their approach to EHR training with the goal of elevating clinician satisfaction, well-being, and overall organizational effectiveness, this article offers four essential takeaways from the enlightening webinar.
1. The experience with initial EHR education is critical to clinicians’ overall satisfaction.
First impressions are everything — even (and especially) when it comes to EHR training and onboarding. Data suggests that use of a certain EHR vendor doesn’t guarantee user satisfaction. So, if it’s not the vendor creating this varying experience, what is it?
KLAS dove deeper into the connection between EHR experience and EHR education. Using a Likert scale, KLAS measured how well initial EHR education prepared clinicians to use the EHR. Correlating those responses with a user’s Net EHR Experience Score (ranging from -100 to +100), users who strongly agree that their initial training prepared them well score 78.0, whereas users who strongly disagree that their initial training prepared them well score a -17.3. This revealed a 95-point difference in user satisfaction — just based on initial training! That difference reveals a major opportunity for improvement.
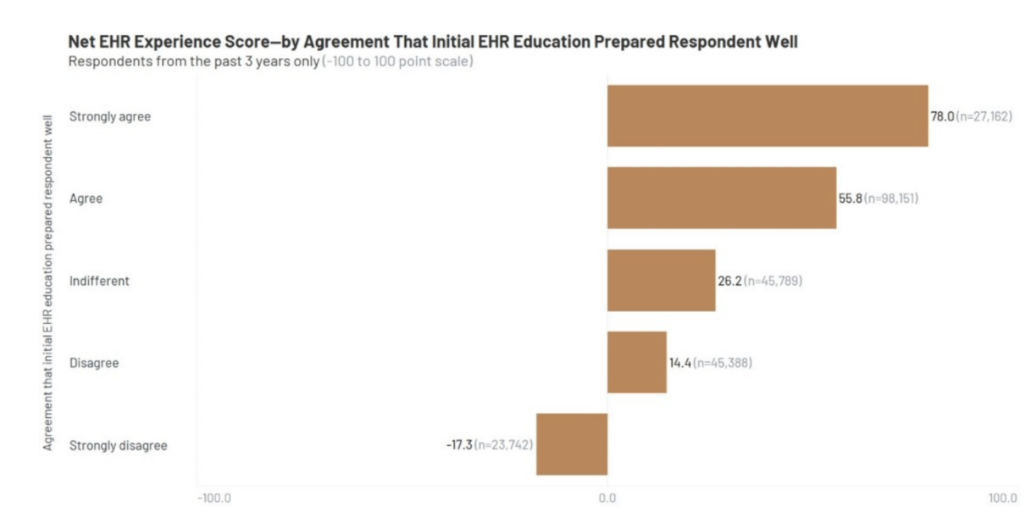
2. Clinicians want more training! But there’s a catch.
To the survey question asking respondents if they want more EHR training, over half said they do! As surprising as it is to see that result, it comes with a big catch. It’s likely that of the clinicians who responded “yes” to more training, they aren’t imagining signing up for more timein a classroom.
In other words, more training doesn’t mean longer training. More training means more high-quality training. As a follow-up to this survey, Jenna Anderson, strategy and operations director from KLAS Arch Collaborative, shared provider feedback about what kind of training they wanted more of. Responses included: “better training up front and subsequently,” “more videos,” “improved specialty-focused training,” and “better access to training materials.”
If an organization’s training is not meeting clinicians where they are, it doesn’t mean training doesn’t work. It means training needs to be better, because clinicians want effective, efficient training. This also applies to the 46% of respondents who replied that they didn’t want more training, assuming the training experience was lacking to them in some way.
3. Online learning that prioritizes science-based retention methods is the biggest differentiator in terms of time savings.
Data indicates that self-directed eLearning has the biggest impact on time savings (above other forms like virtual instructor-led training or classroom training), but when powered by brain science-based methodology, it boosts results.
KLAS data indicates that 91 EHR minutes are saved per week for every one hour of training with self-directed eLearning, whereas the next closest category, in-person one-on-one training saves just 72 minutes. EHR minutes saved are minutes given back to the clinician to focus on what they want to do most: provide high-quality care.

image: https://klasresearch.com/archcollaborative/report/clinician-training-2023/480
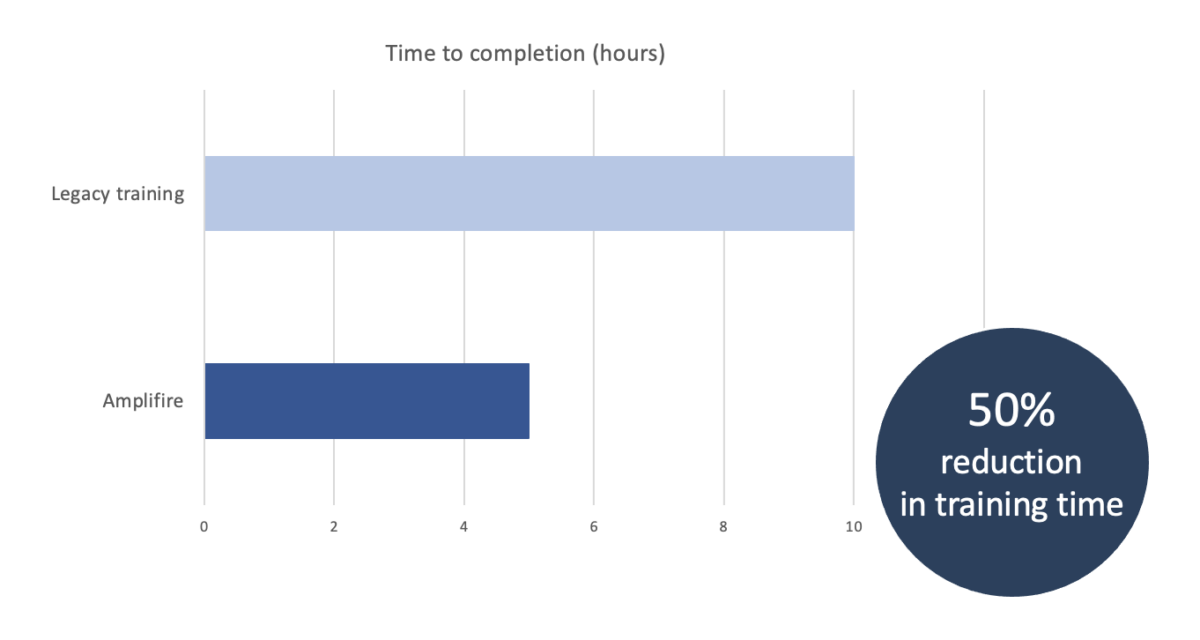
When this self-directed eLearning takes the form adaptive, personalized learning powered by brain science-based learning methodology, it cuts training time even more, targets knowledge gaps, and ensures proficiency, translating to even less time spent in the EHR. For FroedtertHealth, who used self-paced online learning via LMS, switching to adaptive online learning shaved an additional 50% from training time, getting clinicians back on the floor faster, helpingmore patients, and logging more billable hours. This also ties right back to the fact that clinicians want more training. If training is personalized and adapts to each learner’s needs, they learn only what they don’t already know, maximizing training efficacy and boosting the clinician experience by not wasting their time.
4. Robust data and learner insights impact clinician satisfaction and well-being.
Robust learner analytics are the key to doubling down on learning personalization and training optimization. When organizations have access to hidden insights, such as pinpointed knowledge gaps, learner struggle, and confidently held misinformation, they can create individualized remediation plans for specific learners — getting them the coaching they need, sooner.
But deep insights like this help health systems optimize their training program at large. Learner insights reveal what prior knowledge their learners have, allowing them potentially place learners on different tracks. For example, Froedtert Health’s learner data pinpointed consistently low levels of struggle among certain clinicians, so those clinicians are placed on an accelerated plan, thus saving time while respecting learners’ expertise. For clinicians that demonstrated high struggle levels, they are placed on a supportive track to ensure they get the learning they need to be highly proficient. This is different than simply asking if clinicians have prior experience with a particular EHR vendor — some clinicians that indicate that they do have prior experience still demonstrate high levels of struggle. In that case, they will get the support they need (that they may not have otherwise gotten without the deep learner data). From identifying incoming clinician learning trends, they refine their training program to ensure efficiency and efficacy to boost clinician satisfaction. With a training program that is rigorously personalized to clinicians’ needs, their well-being improves. They get the training they want and the learning they need, right when they need it.
This webinar shed light on effective strategies to improve the EHR experience and, by extension, clinician satisfaction. With key takeaways, including the critical role of initial EHR education, the need for more efficient and personalized training, the time-saving potential of self-directed eLearning, and the power of robust learner insights, healthcare systems have the tools to revolutionize their approach. To delve deeper into these insights and elevate clinician satisfaction and organizational effectiveness, watch the full webinar.







